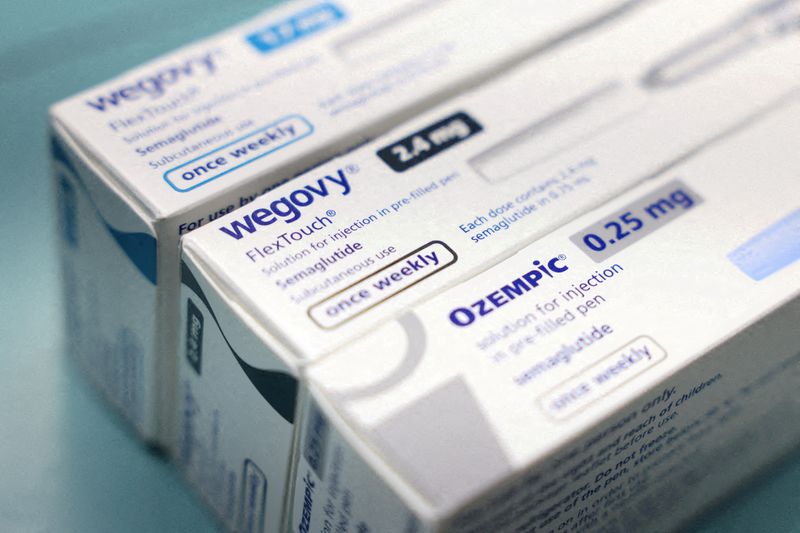
Why Most U.S. Patients Abandon Novo Nordisk’s Wegovy & Ozempic for Weight Loss: A Financial and Health Impact Analysis
By Chad Terhune
Overview
Recent data reveals that only one in four U.S. patients prescribed Novo Nordisk’s Wegovy or Ozempic for weight loss continue these medications after two years. This trend, uncovered through an analysis of U.S. pharmacy claims, has significant implications for patients, healthcare providers, and financial stakeholders alike.
Key Findings
- Patient Adherence: Only 25% of patients adhered to their Wegovy or Ozempic prescriptions after two years, down from 32% after one year.
- Rising Costs: GLP-1 receptor agonists like Wegovy and Ozempic can cost more than $1,000 per month, raising concerns about their long-term affordability.
- Healthcare Impact: If half of U.S. adults with obesity used these drugs, it could cost $411 billion annually, surpassing the total spent on all prescription drugs in 2022 by $5 billion.
Detailed Analysis
Prime Therapeutics and Magellan Rx Management analyzed pharmacy and medical claims data from 3,364 individuals with commercial health plans covering GLP-1 drugs. The study included patients diagnosed with obesity or a body mass index (BMI) of 30 or higher, who received new prescriptions between January and December 2021.
Patient Persistence Over Time
- Wegovy: 24.1% of patients continued without a gap of 60 days or more after two years, down from 36% after one year.
- Ozempic: 22.2% continued after two years, down from 47.1% after one year.
- Saxenda: Only 7.4% remained on this older GLP-1 drug after two years.
Medication Switching and Supply Issues
- Switching Drugs: 26% of patients switched GLP-1 medications during treatment, likely due to supply shortages or changes in insurance coverage.
- Supply Challenges: Both Novo Nordisk and Eli Lilly have struggled to meet the unprecedented demand for these new medications.
Implications for Stakeholders
Patients
Patients face a dilemma when it comes to the long-term use of these medications. Side effects such as nausea and vomiting, high out-of-pocket costs, and the potential for weight regain after stopping the medication are significant concerns.
Employers and Health Plans
Employers and health plans are caught between wanting to provide effective obesity care and managing the financial sustainability of covering these high-cost drugs.
Government and Policymakers
The potential $411 billion annual cost for widespread use of these drugs has drawn criticism from public officials, including President Joe Biden. This raises questions about the cost-effectiveness and long-term sustainability of such treatments within public health plans.
Conclusion
The steady decline in patient persistence with Wegovy and Ozempic highlights critical financial and health challenges. To mitigate these issues, stakeholders must consider the balance between the benefits of weight loss and the economic impact of long-term medication use.
Simplified Breakdown
- What’s Happening?
- Only 1 in 4 patients continue using Wegovy or Ozempic after two years.
- These medications are expensive, costing over $1,000 per month.
- Why Does This Matter?
- If many people used these drugs, it could cost the U.S. $411 billion yearly, more than all other prescription drugs combined.
- High costs and side effects lead many patients to stop using these drugs.
- Who’s Affected?
- Patients: Face high costs and side effects.
- Employers: Struggle with the cost of providing these drugs to employees.
- Government: Potentially huge financial burden on public health plans.
- What Should You Do?
- If considering these medications, discuss the long-term financial and health implications with your doctor.
- Employers and policymakers should evaluate the cost-benefit ratio of covering these drugs.
By understanding these dynamics, you can make more informed decisions about weight-loss treatments and their impact on your finances and health.
- What’s Happening?